Fetal Pacemaker Ready for Human Trial
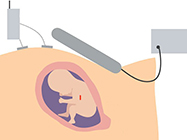
It’s the ultimate MacGyver challenge: Fit a sterile, rechargeable electrode through a hollow tube, just 3.8 millimeters wide, to implant the device in a delicate soft tissue without causing damage. The technology must be both simple and inexpensive to build.
Oh, and the survival of a fetus depends on it.
Such was the challenge undertaken by two doctors and an engineer at the University of Southern California, Los Angeles, about five years ago. This month, the team published details of the recharging system designed for the completed fetal micropacemaker, and they are now prepared to use it in the first human patient.
About 500 fetuses per year are diagnosed with a rare condition in which the heart beats too slowly to pump sufficient blood to the tiny, developing body. A pacemaker could be used to control that abnormal heart rhythm, yet attempts to place an adult pacemaker in the mother and attach its electrical lead to the unborn child have failed, because the fetus often changes position and pulls out the lead.
The condition begins to impact the health of a fetus about 28 weeks into a pregnancy. Loeb, working alongside cardiologist Yaniv Bar-Cohen of Children’s Hospital Los Angeles and Ramen Chmait, director of the Fetal Surgery Program at the USC Keck School of Medicine, developed and tested a device that could be implanted during that timeframe.
The micropacemaker, made of only 7 components, is a slim cylinder designed to fit through the diameter of a 3.8 mm insertion cannula, a hollow implantation tool used in fetal surgeries. The pacemaker itself is “actually very retro in its design,” says Loeb. It relies upon techniques used in the first cardiac pacemakers from the 1950s, such as a simple circuitry—a single transistor relaxation oscillator—and an epoxy capsule. Current adult pacemakers rely on longer-lasting titanium instead of epoxy, yet the fetal pacemaker needs to function for only several months, and titanium was too bulky to fit through the cannula, says Loeb.
For more details: -http://googleweblight.com/i?u=http://spectrum.ieee.org/the-human-os/biomedical/devices/fetal-pacemaker-ready-for-human-trial&hl=en-IN





























